Introduction
Proper phlebotomy practice is the foundation of accurate laboratory diagnostics. A significant percentage of laboratory errors occur during the pre-analytical phase, particularly during blood collection. Therefore, correct selection of collection tubes, devices, needle gauge, fill volume, and mixing technique is essential.
This comprehensive guide provides a structured explanation of blood collection systems and tubes, aligned with NABL and CAP quality standards. It is suitable for use as a laboratory reference blog or training material.
𝟏. 𝐁𝐥𝐨𝐨𝐝 𝐂𝐨𝐥𝐥𝐞𝐜𝐭𝐢𝐨𝐧 𝐒𝐲𝐬𝐭𝐞𝐦𝐬
Blood collection systems are classified into:
Vacutainer (Vacuum) System
Non-Vacuum (Syringe) System
Both systems can use tubes with or without anticoagulants.
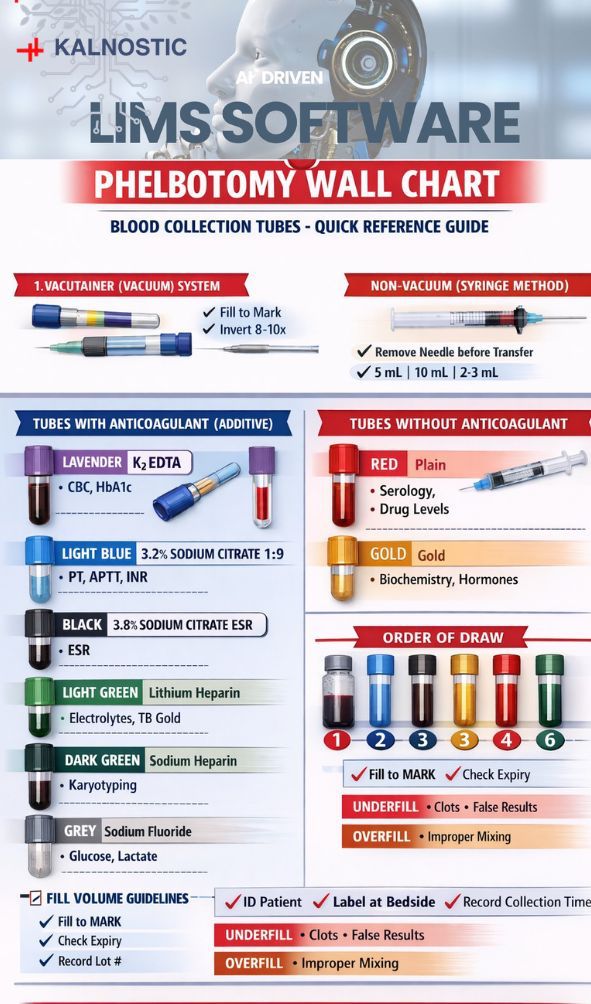
𝐈. 𝐕𝐚𝐜𝐮𝐭𝐚𝐢𝐧𝐞𝐫 (𝐕𝐚𝐜𝐮𝐮𝐦) 𝐒𝐲𝐬𝐭𝐞𝐦
𝐖𝐡𝐚𝐭 𝐢𝐬 𝐚 𝐕𝐚𝐜𝐮𝐭𝐚𝐢𝐧𝐞𝐫?
A vacutainer tube is a sterile blood collection tube containing a pre-calibrated vacuum. When connected to a double-ended needle and holder, the vacuum automatically draws a fixed volume of blood into the tube.
𝐀𝐝𝐯𝐚𝐧𝐭𝐚𝐠𝐞𝐬
Ensures accurate blood-to-additive ratio
Closed system (reduces contamination risk)
Lower hemolysis risk
Faster multi-tube collection
Preferred system under NABL and CAP guidelines
𝐂𝐨𝐥𝐥𝐞𝐜𝐭𝐢𝐨𝐧 𝐃𝐞𝐯𝐢𝐜𝐞𝐬 𝐔𝐬𝐞𝐝
Vacutainer holder (adapter)
Double-ended multisample needle
𝐑𝐞𝐜𝐨𝐦𝐦𝐞𝐧𝐝𝐞𝐝 𝐍𝐞𝐞𝐝𝐥𝐞 𝐒𝐩𝐞𝐜𝐢𝐟𝐢𝐜𝐚𝐭𝐢𝐨𝐧𝐬
For Adults (routine):
21 Gauge
1–1.5 inch length
For small or fragile veins:
22 Gauge
For pediatric patients:
23 Gauge butterfly needle
Using very small gauge needles (e.g., 25G) may increase hemolysis risk.
𝐈𝐈. 𝐍𝐨𝐧-𝐕𝐚𝐜𝐮𝐮𝐦 (𝐒𝐲𝐫𝐢𝐧𝐠𝐞) 𝐒𝐲𝐬𝐭𝐞𝐦
𝐖𝐡𝐚𝐭 𝐢𝐬 𝐚 𝐍𝐨𝐧-𝐕𝐚𝐜𝐮𝐮𝐦 𝐓𝐮𝐛𝐞?
Non-vacuum tubes do not contain negative pressure. Blood is drawn manually using a syringe and then transferred into the tube.
𝐖𝐡𝐞𝐧 𝐢𝐬 𝐢𝐭 𝐔𝐬𝐞𝐝?
Difficult venous access
Pediatric patients
Geriatric patients
Collapsible veins
𝐂𝐨𝐥𝐥𝐞𝐜𝐭𝐢𝐨𝐧 𝐃𝐞𝐯𝐢𝐜𝐞𝐬 𝐔𝐬𝐞𝐝
Sterile disposable syringe
Needle attached to syringe
𝐑𝐞𝐜𝐨𝐦𝐦𝐞𝐧𝐝𝐞𝐝 𝐒𝐲𝐫𝐢𝐧𝐠𝐞 𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐢𝐞𝐬
Routine investigations: 5 mL
Multiple investigations: 10 mL
Pediatric cases: 2–3 mL
𝐑𝐞𝐜𝐨𝐦𝐦𝐞𝐧𝐝𝐞𝐝 𝐍𝐞𝐞𝐝𝐥𝐞 𝐆𝐚𝐮𝐠𝐞
Adults: 21G or 22G
Pediatrics: 23G
𝐈𝐦𝐩𝐨𝐫𝐭𝐚𝐧𝐭 𝐏𝐫𝐞𝐜𝐚𝐮𝐭𝐢𝐨𝐧𝐬:
Remove the needle before transferring blood into the tube.
Do not forcefully push blood into tubes.
Avoid frothing or hemolysis.
2. 𝐂𝐥𝐚𝐬𝐬𝐢𝐟𝐢𝐜𝐚𝐭𝐢𝐨𝐧 𝐨𝐟 𝐁𝐥𝐨𝐨𝐝 𝐂𝐨𝐥𝐥𝐞𝐜𝐭𝐢𝐨𝐧
Tubes are divided into:
A. Tubes with Anticoagulants (Additives)
B. Tubes without Anticoagulants
A. 𝐓𝐮𝐛𝐞𝐬 𝐰𝐢𝐭𝐡 𝐀𝐧𝐭𝐢𝐜𝐨𝐚𝐠𝐮𝐥𝐚𝐧𝐭𝐬
These tubes prevent clotting and are used when plasma or whole blood is required.
1. 𝐓𝐡𝐞 𝐋𝐚𝐯𝐞𝐧𝐝𝐞𝐫 𝐓𝐨𝐩 (𝐄𝐃𝐓𝐀 𝐓𝐮𝐛𝐞)
This is the workhorse of the hematology lab. It contains EDTA (Ethylenediaminetetraacetic acid), which acts as a powerful anticoagulant by binding calcium in the blood. This keeps the blood in its liquid state and preserves the shape of the blood cells.
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞:Potassium EDTA
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞:
Whole blood
EDTA plasma
𝐂𝐨𝐦𝐦𝐨𝐧 𝐔𝐬𝐞𝐬:
Complete Blood Count (CBC)
Peripheral smear
HbA1c
Blood grouping
𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐲: Ranges from 2.0 mL to 4.0 mL.
𝐓𝐡𝐞 𝐃𝐞𝐦𝐚𝐫𝐜𝐚𝐭𝐢𝐨𝐧: Indicated by a black or white line on the label.
𝐅𝐢𝐥𝐥 𝐑𝐞𝐪𝐮𝐢𝐫𝐞𝐦𝐞𝐧𝐭:
Must be filled up to the manufacturer’s indicated mark (commonly 2–3 mL).
If Underfilled:
Excess EDTA relative to blood
RBC shrinkage
False low hematocrit
If Overfilled:
Risk of clot formation
2. 𝐋𝐢𝐠𝐡𝐭 𝐁𝐥𝐮𝐞 𝐓𝐨𝐩 – 𝟑.𝟐% 𝐒𝐨𝐝𝐢𝐮𝐦 𝐂𝐢𝐭𝐫𝐚𝐭𝐞
This tube contains Sodium Citrate, a reversible anticoagulant. It’s used specifically for coagulation studies because it preserves the clotting factors in the plasma. The ratio of blood to additive is critical here, which is why these tubes must be filled to the exact line.
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞:3.2% Sodium Citrate
Required Ratio: 1 part citrate : 9 parts blood
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞:Citrated plasma
𝐂𝐨𝐦𝐦𝐨𝐧 𝐔𝐬𝐞𝐬:
PT
INR
APTT
D-dimer
𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐲: Usually 1.8 mL or 2.7 mL.
𝐓𝐡𝐞 𝐃𝐞𝐦𝐚𝐫𝐜𝐚𝐭𝐢𝐨𝐧: This is the most “diva” tube in the lab. It requires a strict 9:1 ratio (9 parts blood to 1 part citrate).
𝐂𝐫𝐢𝐭𝐢𝐜𝐚𝐥 𝐍𝐨𝐭𝐞:
This tube must be filled exactly to the indicated level.
If Underfilled:
Excess anticoagulant
Falsely prolonged PT/APTT
If Overfilled:
Clot formation risk
Strict adherence to fill volume is mandatory under CAP standards.
3. 𝐋𝐢𝐠𝐡𝐭 𝐆𝐫𝐞𝐞𝐧 𝐓𝐨𝐩 – 𝐋𝐢𝐭𝐡𝐢𝐮𝐦 𝐇𝐞𝐩𝐚𝐫𝐢𝐧
Green tubes contain Heparin (sodium, lithium, or ammonium). Heparin works by inhibiting thrombin, preventing the blood from clotting. This allows for “whole blood” or plasma testing.
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞: Lithium Heparin
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞: Plasma
𝐂𝐨𝐦𝐦𝐨𝐧 𝐔𝐬𝐞𝐬:
Electrolytes
Liver Function Test (LFT)
Renal Function Test (RFT)
Emergency chemistry
𝐒𝐩𝐞𝐜𝐢𝐚𝐥 𝐔𝐬𝐞:
TB Gold testing (Interferon Gamma Release Assay type investigations)
Allows rapid plasma separation.
𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐲: 2.0 mL to 6.0 mL.
𝐓𝐡𝐞 𝐌𝐢𝐧𝐢𝐦𝐮𝐦: Ideally half-full.
4. 𝐆𝐫𝐞𝐲 𝐓𝐨𝐩 – 𝐒𝐨𝐝𝐢𝐮𝐦 𝐅𝐥𝐮𝐨𝐫𝐢𝐝𝐞
If a lab needs to check your blood sugar levels from hours ago, they use the grey tube. It contains Sodium Fluoride and Potassium Oxalate. The fluoride acts as an “antiglycolytic” agent—it stops the red blood cells from eating the glucose in the tube, ensuring the sugar level remains stable for measurement.
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞:Sodium Fluoride with Potassium Oxalate
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞: Plasma
𝐂𝐨𝐦𝐦𝐨𝐧 𝐔𝐬𝐞𝐬:
Blood glucose
Lactate
𝐅𝐮𝐧𝐜𝐭𝐢𝐨𝐧:
Prevents glycolysis by inhibiting enzymatic activity.
𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐲: 2.0 mL to 4.0 mL.
𝐓𝐡𝐞 𝐌𝐢𝐧𝐢𝐦𝐮𝐦: 75% full is the standard.
5. 𝐁𝐥𝐚𝐜𝐤 𝐓𝐨𝐩 – 𝟑.𝟖% 𝐒𝐨𝐝𝐢𝐮𝐦 𝐂𝐢𝐭𝐫𝐚𝐭𝐞 (𝐄𝐒𝐑 𝐓𝐮𝐛𝐞)
The Black tube is a bit of a specialist. It contains a Buffered Sodium Citrate solution. While this sounds similar to the Light Blue tube, the concentration and ratio of anticoagulant to blood are different (usually a 1:4 ratio in the black tube vs. 1:9 in the blue).
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞: 3.8% Sodium Citrate
Required Ratio: 1 part citrate : 4 parts blood
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞: Whole blood
𝐏𝐫𝐢𝐦𝐚𝐫𝐲 𝐔𝐬𝐞:
Erythrocyte Sedimentation Rate (ESR)
Types Available:
Standard ESR tube
Long automated ESR tube (used in automated ESR analyzers; compatible with Westergren method)
𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐲: Usually 1.28 mL or 2.0 mL.
𝐓𝐡𝐞 𝐃𝐞𝐦𝐚𝐫𝐜𝐚𝐭𝐢𝐨𝐧: Extremely precise.
If incorrect volume is collected, ESR values may be falsely altered.
𝐁. 𝐓𝐮𝐛𝐞𝐬 𝐖𝐢𝐭𝐡𝐨𝐮𝐭 𝐀𝐧𝐭𝐢𝐜𝐨𝐚𝐠𝐮𝐥𝐚𝐧𝐭
𝟏. 𝐑𝐞𝐝 𝐓𝐨𝐩 – 𝐏𝐥𝐚𝐢𝐧 𝐓𝐮𝐛𝐞
Think of this as the “plain” tube. It usually contains no additive or a clot activator. It allows the blood to clot naturally, separating the liquid serum from the solid cells.
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞: None
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞: Serum
𝐂𝐨𝐦𝐦𝐨𝐧 𝐔𝐬𝐞𝐬:
Serology
Drug level monitoring
Hormone assays
𝐏𝐫𝐨𝐜𝐞𝐝𝐮𝐫𝐞:
Allow blood to clot for approximately 30 minutes before centrifugation.
𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐲: 3.5 mL to 10.0 mL.
𝐓𝐡𝐞 𝐌𝐢𝐧𝐢𝐦𝐮𝐦: These are the most flexible. As long as there is enough serum to run the specific test (usually 1 mL of serum requires about 2 mL of whole blood), the lab can usually process it.
𝐎𝐫𝐝𝐞𝐫 𝐨𝐟 𝐃𝐫𝐚𝐰 (𝐒𝐭𝐚𝐧𝐝𝐚𝐫𝐝 𝐏𝐫𝐚𝐜𝐭𝐢𝐜𝐞)
Blood Culture
Light Blue (3.2% Citrate)
Serum Tubes (Red / Yellow)
Green (Heparin)
Lavender (EDTA)
Grey (Fluoride)
Black (ESR)
Following the correct order prevents additive carryover contamination.
2. 𝐑𝐞𝐝/𝐎𝐫𝐚𝐧𝐠𝐞 𝐓𝐨𝐩 – 𝐂𝐥𝐨𝐭 𝐀𝐜𝐭𝐢𝐯𝐚𝐭𝐨𝐫 𝐓𝐮𝐛𝐞
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞: Silica clot activator
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞: Serum
𝐂𝐨𝐦𝐦𝐨𝐧 𝐔𝐬𝐞𝐬:
Routine biochemistry
Immunology
Hormone assays
Speeds up clot formation.
3.𝐘𝐞𝐥𝐥𝐨𝐰/𝐆𝐨𝐥𝐝 𝐓𝐨𝐩 – 𝐆𝐞𝐥 + 𝐂𝐥𝐨𝐭 𝐀𝐜𝐭𝐢𝐯𝐚𝐭𝐨𝐫 (𝐒𝐞𝐫𝐮𝐦 𝐒𝐞𝐩𝐚𝐫𝐚𝐭𝐨𝐫 𝐓𝐮𝐛𝐞 – 𝐒𝐒𝐓)
𝐀𝐝𝐝𝐢𝐭𝐢𝐯𝐞: Clot activator + gel separator
𝐒𝐚𝐦𝐩𝐥𝐞 𝐓𝐲𝐩𝐞: Serum
𝐂𝐨𝐦𝐦𝐨𝐧 𝐔𝐬𝐞𝐬:
Biochemistry
Hormones
Tumor markers
Serology
After centrifugation, the gel forms a barrier between serum and cells, improving sample stability.
𝐂𝐚𝐩𝐚𝐜𝐢𝐭𝐲: 3.5 mL to 10.0 mL.
𝐓𝐡𝐞 𝐌𝐢𝐧𝐢𝐦𝐮𝐦: These are the most flexible. As long as there is enough serum to run the specific test (usually 1 mL of serum requires about 2 mL of whole blood), the lab can usually process it.
𝐃𝐢𝐝 𝐘𝐨𝐮 𝐊𝐧𝐨𝐰?
The ACD Yellow Top is usually the first tube drawn after blood cultures. This is because we want the “freshest” possible cells for genetic testing before other anticoagulants like EDTA (Lavender) or Heparin (Green) are introduced, which can occasionally interfere with sensitive DNA amplification processes like PCR.
𝟒. 𝐅𝐢𝐥𝐥 𝐕𝐨𝐥𝐮𝐦𝐞 𝐆𝐮𝐢𝐝𝐞𝐥𝐢𝐧𝐞𝐬
Each manufacturer calibrates tubes differently (2 mL, 3 mL, 4 mL, etc.).
Always:
Fill to the indicated mark
Check expiry date
Verify lot number
Perform 8–10 gentle inversions for additive tubes
If Underfilled:
Incorrect blood-to-additive ratio
Clot formation
Inaccurate test results
If Overfilled:
Incomplete anticoagulation
Invalid results
𝐖𝐡𝐲 𝐏𝐫𝐨𝐩𝐞𝐫 𝐓𝐮𝐛𝐞 𝐒𝐞𝐥𝐞𝐜𝐭𝐢𝐨𝐧 𝐌𝐚𝐭𝐭𝐞𝐫𝐬
Using the wrong tube can:
Alter test results
Cause sample rejection
Delay diagnosis
Require recollection
Each additive interacts differently with blood components, so correct selection ensures accuracy, reliability, and patient safety.
𝟓. 𝐐𝐮𝐚𝐥𝐢𝐭𝐲 𝐚𝐧𝐝 𝐒𝐚𝐟𝐞𝐭𝐲 𝐑𝐞𝐪𝐮𝐢𝐫𝐞𝐦𝐞𝐧𝐭𝐬 (𝐍𝐀𝐁𝐋 & 𝐂𝐀𝐏 𝐂𝐨𝐦𝐩𝐥𝐢𝐚𝐧𝐜𝐞)
Proper patient identification
Bedside labeling
Documentation of collection time
Monitoring of sample rejection criteria
Control of hemolysis rates
Staff training and competency assessment
Proper storage and transport conditions
𝐂𝐨𝐧𝐜𝐥𝐮𝐬𝐢𝐨𝐧
Accurate laboratory diagnosis begins with correct phlebotomy practice. Selecting the proper tube, using the correct collection device, maintaining the correct fill volume, and following the appropriate order of draw are critical steps in ensuring reliable laboratory results.
Adhering to NABL and CAP standards minimizes pre-analytical errors, enhances patient safety, and ensures quality laboratory services.